Sam Brusco, Associate Editor04.03.17
A new brand of philanthropy, Beyond Type 1 harnesses the power of social media and technology to change what it means to live with type 1 diabetes. Its founders consist of varying degrees of celebrities who have the disease or have children who do: Juliet de Baubigny, a partner at Kleiner Perkins Caulfield & Byers whose son was diagnosed in 2012; Sarah Lucas, Beyond Type 1’s CEO, event designer, writer, and lifestyle expert whose daughter was diagnosed in 1998; Sam Talbot, a chef, restaurant owner, and Top Chef competitor named “fan favorite” who was diagnosed at age 12; and—most prominently—Nick Jonas, multi-platinum recording artist and actor, who was diagnosed at age 13. (Jonas is a current user and advocate for Dexcom, a company that develops continuous glucose monitors.)
Beyond Type 1 is a registered 501(c)3, and aims to educate the global community about the chronic autoimmune disease, and also provides resources and support for those who are living with type 1 diabetes.
The vast network of support Beyond Type 1 offers those struggling with the disease a wealth of information about strategies to manage their diabetes, and even thrive despite it. The Beyond Type 1 app links 12,000 members from 100 different countries to share stories, read accounts from the community, ask questions, participate in polls, troubleshoot, and be part of a community that offers inspiration and support. Beyond Type 1 also campaigns to spread awareness and change current misconceptions of the disease through Type 1 educational resources, which include printed materials, a PowerPoint presentation outlining treatment and naming celebrities with the disease, and the #LivingBeyond session for Type 1 diabetes camps.
“What intrigued me about Beyond Type 1 is the fact that it’s such a contemporary organization—that’s dealing with social media in a very effective and more productive way than some of the other organizations, (every one of them being important and great),” Victor Garber, a Canadian actor and singer diagnosed with type 1 diabetes at age 12, told Beyond Type 1 in an interview. “But this one resonated with me because of how many young kids are dealing with this, and young kids are on social media. [An online community] can be a very powerful tool in dealing with any disease.”
However, participation in a community, while useful and inspirational, is only the first step in proactive diabetes management. For patients to truly thrive in spite of the disease, there are a few loops in care that digital health technologies can help to close.
Closing the Treatment Loop
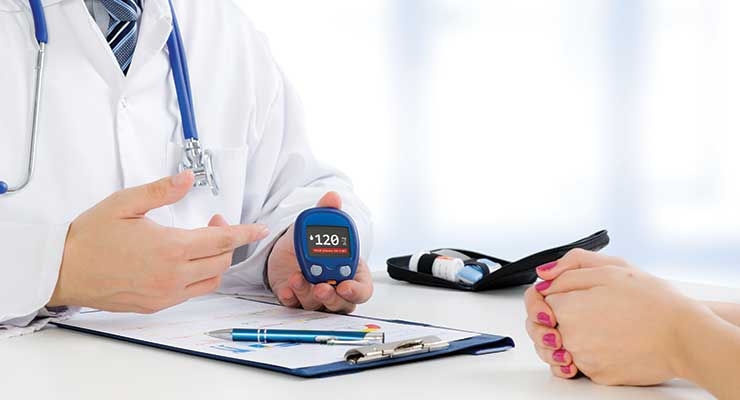
Living with diabetes—especially type 1 diabetes—is an endless cycle of remembrance. Patients must remember to check glucose levels multiple times a day to prevent hyperglycemic attacks while monitoring insulin doses to prevent hypoglycemic attacks. Exercise is also important for proper diabetes care; being active aids blood glucose level stabilization. Adequate nutrition is perhaps the most important management aspect to control, and is unfortunately the most difficult to regulate. Understanding how different diets affect blood glucose and developing solid meal plans will be crucial to a management plan.
These regimens are typically part of a treatment plan developed with a healthcare team. That treatment plan involves selecting the insulin (or insulins) optimal for the patient, and forging an exercise routine and nutrition plan. Then, because diabetes is an incredibly dynamic disease state, patients will have to do it all over again in a few months once their doctor assesses how effective the current plan has been. Usually, these tweaks in treatment occur every two to three months (more or less depending on the patient’s health) in the form of a 10-minute consultation. During this time, doctors review patient history and update the plan, and the cycle begins anew. Unfortunately, this method isn’t scalable in the current healthcare environment—there are simply too many patients and too few clinicians to give each diabetic patient the personalized attention they require.
In order to close the “treatment loop” that can occur between doctor and patient as a result of inadequate consultation time, communication, and real-time health data, many patients are using mobile health (mHealth) solutions to more effectively and efficiently manage their diabetes. For those who aren’t up to speed on what mHealth entails, as described by the eponymous mHealth Alliance: “mHealth stands for mobile-based or mobile-enhanced solutions that deliver health. The ubiquity of mobile devices in the developed or developing world presents the opportunity to improve health outcomes through the delivery of innovative medical and health services with information and communication technologies to the farthest reaches of the globe.”
mHealth management leverages cell phones or other wirelessly connected devices to connect doctor and patient in order to develop a “hybrid” treatment plan—a combination of self-management by the patient and guidance from the healthcare professional. It’s typically combined with some sort of hardware—in the case of diabetes, a glucose monitor and insulin delivery device—then records actionable data, which is wirelessly transmitted to a clinician. If the data reveals a trend toward unhealthy diabetes management, healthcare professionals can notice it right away and update the patient’s treatment plan, without an appointment.
If this is all sounding a bit esoteric, perhaps an illustration of such management technologies would help to illuminate its practicality.
The Israeli startup GlucoMe, for example, combines cloud-based data analysis and stripped-down medical hardware in order to better address diabetes management. GlucoMe’s management platform combines a smart glucose monitor, an insulin pen monitor, a mobile app, and a cloud-based management system to help streamline treatment. GlucoMe’s “Digital Diabetes Clinic” leverages all the patient’s data gained from continuous use of the platform in order to recommend treatment programs for individuals, as well as manage larger populations of diabetics.
The monitor still uses a lancing device to measure blood glucose, but also analyzes it and communicates the information to the user’s smartphone via the company’s acoustic data transfer system. The data transfer doesn’t rely on WiFi or cellular data, enabling use of the platform in more remote areas. The system then relays the information to a healthcare professional, along with a recommended treatment plan.
“We won’t just tell you this patient is in a high glucose condition or a low glucose condition,” Ben Aharon, founder and CEO of GlucoMe, said in an interview with The Times of Israel. “It will analyze the data and recommend a full treatment plan.”
While the platform will be quite beneficial for individual patients and their practitioners to better manage treatment plans, the company’s hardware is only an enabler for data collection, according to Aharon. The cloud-based system could be used to more aptly manage diabetic populations like those receiving treatment at a single clinic, or everyone with the disease in a specific region. Algorithms and machine learning strategies can then be shared with healthcare providers to determine which patients may need further attention. The technology’s aim here is to discover which patients may only need digital intervention (like minor adjustments to medication plans), and which may need to physically see their healthcare provider—culminating in efficiency for clinicians and improving treatment for patients.
Thus far, GlucoMe has completed trials in the United States, Germany, and Israel, was awarded CE mark clearance in August 2016, and expects to win U.S. Food and Drug Administration (FDA) clearance this year.
Type 1 diabetes (as evidenced by the name) isn’t the only form of the disease, of course—it just presents more of a management challenge due to insulin dependency. In fact, 95 percent of diabetic patients have type 2 diabetes,1 and don’t necessarily require comprehensive management platforms like GlucoMe. Livongo Health (a consumer digital health company focused on chronic conditions), partnered with Voluntis (a company that develops therapeutic companion software with a focus on managing chronic conditions) in February to develop an insulin titration app that recommends basal insulin doses for patients with type 2 diabetes. Livongo’s cellular-enabled blood glucose meter leverages data science to provide personal insights and coaching based on real-time information. Combining this with Voluntis’ Insulia—which delivers automated basal insulin dose recommendations and educational coaching messages through a smartphone app—seeks to improve medication adherence and optimize management. That way, patients can avoid the potential adverse health effects arising from suboptimal medication use.
Closing the Technology Loop
The be all and end all of type 1 diabetes management technology is widely regarded to be something called a “closed loop system”—an automatic control system in which an operation, process, or mechanism is regulated by continuous feedback. In the context of diabetes, that continuous feedback takes the form of a continuous glucose monitor (CGM), such as those included in Dexcom’s G5 Mobile CGM System, Animas’ Vibe System, or Medtronic plc’s MiniMed series. To complete the analogy, the operation, process, or mechanism to be regulated would be the frequency and amount of insulin delivered by a pump, based on the CGM’s blood glucose readings.
So rather than patients sticking themselves multiple times a day to determine proper insulin dosage, a closed loop system does (most of) the work of measuring and dosing. Of course, the system can’t yet account for things like deviance in diet or exercise (which the patient would still have to input into the system) but it removes a great deal of the burden of responsibility for diabetic patients.
“The development of the MiniMed 670G system was motivated by our desire to help patients achieve better health and greater freedom,” explained Mike Hill, vice president of global marketing for intensive insulin management at global medical technology company Medtronic. “People with diabetes spend a significant amount of time managing their disease on a daily basis. While this doesn’t prohibit patients from living a normal life, it can be quite burdensome—mentally, physically, and emotionally. This latest advancement demonstrates our commitment to both improving clinical outcomes as well as simplifying diabetes management to improve quality of life. This is all made possible by the advancements made to our smart algorithms that enable greater glucose control with reduced patient input.”
Medtronic’s MiniMed 670G system, dubbed the world’s first approved hybrid closed loop system for insulin delivery, won its FDA nod in September 2016. It features an algorithm called SmartGuard HCL (for Hybrid Closed Loop) for therapy customization. Rather than a fully-closed loop system, a hybrid closed loop means the device modulates the user’s basal rate through micro-boluses. Closing this loop greatly reduces the stress on diabetics about figuring out their basal rate—with the technology diabetic patients and providers can focus their efforts on selecting the best level of automation to fit their management plan. The system’s glucose sensor also lasts for seven days, and contains diagnostic technology that monitors the sensor’s health.
“There is much interest among the diabetes community to increase the level of automation of diabetes technology solutions,” observed Hill. Of course, the system isn’t completely automated—patients still need to input certain sets of pertinent external data to ensure the most effective management plan.
“Our MiniMed 670G system, known as a hybrid closed loop system, still requires some interaction on the part of patients. Users of the system will need to enter mealtime carbohydrates, accept bolus correction recommendations, and periodically calibrate the sensor,” he continued. “The next step in our phased approach will focus on advancing our algorithm to enable automated correction boluses. Once this challenge is addressed, we will focus our efforts on automating meal-time boluses. The timing for development will be dependent upon on multiple variables, but we are committed to a phased approach that will increase the system’s ability to further automate certain tasks with the ultimate goal of developing a fully automated, closed loop system.”
Since MiniMed 670G was revealed, many have taken to dubbing the device the “artificial pancreas.” While MiniMed 670G’s intended function is to essentially mimic the function of the pancreas by delivering an insulin dose based on an algorithm derived from the patient’s pattern of blood glucose levels, misperceptions about what the term “artificial pancreas” means might lead to misinterpretations of the device’s function.
“To ensure clarity around Medtronic’s focus, we are moving away from using the term ‘artificial pancreas’ as perceptions around what that means varies,” Hill said. “Our focus is on increasing automation of our advanced insulin pump systems through smart algorithms that reduce the need for patient interaction and decision-making. We are working to transform diabetes care by taking a holistic approach that goes beyond devices, and uses informatics and integrated care to achieve real results for people living with diabetes. We know that every person’s journey with diabetes is unique, so we strive to understand their diverse needs and develop technologies that meet them.”
Of course, the MiniMed 670G isn’t the only device—though it was the first to gain FDA approval—with partial closed-loop capabilities. In December 2016, the FDA also approved the Animas (part of the Johnson & Johnson Diabetes Care companies) OneTouch Vibe insulin pump, which is integrated with Dexcom’s G5 Mobile CGM technology. This system requires a bit more participation on the part of the patient; blood glucose readings are collected by Dexcom’s sensor, sent to the insulin pump’s screen and compatible smart device, and the user is prompted to deliver the precise amount of insulin they would need from the pump.
Animas’ system is, however, the only integrated system approved for children as young as age 2. Parents and caregivers (up to five people in addition to the primary smart device, as specified by Dexcom’s app) can access their child’s blood glucose levels to make treatment choices.
“This system will offer kids living with diabetes a sense of freedom and will provide loved ones and caregivers with an insulin delivery and monitoring system that they can trust,” said John Wilson, worldwide vice president of insulin delivery for Animas Corporation.
Easing the Burden on Patients and Providers
Whether through constant feedback from a support group, a mobile management platform, or a device, closing the loop on care is the most promising avenue to ease the burden of diabetes management. Ideally, each of these tools would come together to form a personalized management plan that attacks the disease on multiple fronts.
Closed-loop technology relieves the burden of multiple daily blood glucose tests, and calculates recommended insulin dose—then either delivers it automatically or prompts initiation by the patient. Integrated management platforms help to close the loop between patients and their healthcare providers, enabling constant communication and transmission of blood glucose data to make tweaks in treatment in near-real-time, instead of through often laborious scheduling of clinic visits. Combining these tools with a network of support such as that provided by Beyond Type 1 or other similar diabetes support groups allows the constant feedback and subsequent adjustment that a true closed-loop system facilitates. All of these proactive tools can ultimately help to lessen the financial burden on patients by reducing the number of emergency visits due to spikes in blood glucose.
“The cost of diabetes to the healthcare system has been rising,” noted Hill. “In fact, the costs associated with hypoglycemia can be sizeable—with a single emergency service totaling $1,387 and a single inpatient service totaling $17,564.”
With digital health tools, anomalies in blood glucose levels could be resolved before they reach the critical point where an emergency room visit becomes necessary. In an ideal situation, there would be multiple lines of defense to prevent that costly trip to the hospital. A closed-loop technology would hopefully catch the anomaly first, administering the necessary amount of insulin to help stabilize glucose levels. The information would then either be communicated to a healthcare professional via the device, or a companion mobile health management tool. A short conversation with a healthcare provider would then determine whether a clinic visit is necessary or a resolution can be achieved from home.
Each of these tools—combined with inclusion in an online community—can converge to form a “closed-loop support system” for diabetes patients. It’s true that diabetes is a chronic condition requiring careful consideration of almost every aspect of the patient’s lifestyle, but it’s one that tens of millions of people manage every day—and those people are happy to loop patients in on the solutions that help them to thrive.
Reference
1 Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. Atlanta, GA: U.S. Department of Health and Human Services; 2014.
Beyond Type 1 is a registered 501(c)3, and aims to educate the global community about the chronic autoimmune disease, and also provides resources and support for those who are living with type 1 diabetes.
The vast network of support Beyond Type 1 offers those struggling with the disease a wealth of information about strategies to manage their diabetes, and even thrive despite it. The Beyond Type 1 app links 12,000 members from 100 different countries to share stories, read accounts from the community, ask questions, participate in polls, troubleshoot, and be part of a community that offers inspiration and support. Beyond Type 1 also campaigns to spread awareness and change current misconceptions of the disease through Type 1 educational resources, which include printed materials, a PowerPoint presentation outlining treatment and naming celebrities with the disease, and the #LivingBeyond session for Type 1 diabetes camps.
“What intrigued me about Beyond Type 1 is the fact that it’s such a contemporary organization—that’s dealing with social media in a very effective and more productive way than some of the other organizations, (every one of them being important and great),” Victor Garber, a Canadian actor and singer diagnosed with type 1 diabetes at age 12, told Beyond Type 1 in an interview. “But this one resonated with me because of how many young kids are dealing with this, and young kids are on social media. [An online community] can be a very powerful tool in dealing with any disease.”
However, participation in a community, while useful and inspirational, is only the first step in proactive diabetes management. For patients to truly thrive in spite of the disease, there are a few loops in care that digital health technologies can help to close.
Closing the Treatment Loop
Living with diabetes—especially type 1 diabetes—is an endless cycle of remembrance. Patients must remember to check glucose levels multiple times a day to prevent hyperglycemic attacks while monitoring insulin doses to prevent hypoglycemic attacks. Exercise is also important for proper diabetes care; being active aids blood glucose level stabilization. Adequate nutrition is perhaps the most important management aspect to control, and is unfortunately the most difficult to regulate. Understanding how different diets affect blood glucose and developing solid meal plans will be crucial to a management plan.
These regimens are typically part of a treatment plan developed with a healthcare team. That treatment plan involves selecting the insulin (or insulins) optimal for the patient, and forging an exercise routine and nutrition plan. Then, because diabetes is an incredibly dynamic disease state, patients will have to do it all over again in a few months once their doctor assesses how effective the current plan has been. Usually, these tweaks in treatment occur every two to three months (more or less depending on the patient’s health) in the form of a 10-minute consultation. During this time, doctors review patient history and update the plan, and the cycle begins anew. Unfortunately, this method isn’t scalable in the current healthcare environment—there are simply too many patients and too few clinicians to give each diabetic patient the personalized attention they require.
In order to close the “treatment loop” that can occur between doctor and patient as a result of inadequate consultation time, communication, and real-time health data, many patients are using mobile health (mHealth) solutions to more effectively and efficiently manage their diabetes. For those who aren’t up to speed on what mHealth entails, as described by the eponymous mHealth Alliance: “mHealth stands for mobile-based or mobile-enhanced solutions that deliver health. The ubiquity of mobile devices in the developed or developing world presents the opportunity to improve health outcomes through the delivery of innovative medical and health services with information and communication technologies to the farthest reaches of the globe.”
mHealth management leverages cell phones or other wirelessly connected devices to connect doctor and patient in order to develop a “hybrid” treatment plan—a combination of self-management by the patient and guidance from the healthcare professional. It’s typically combined with some sort of hardware—in the case of diabetes, a glucose monitor and insulin delivery device—then records actionable data, which is wirelessly transmitted to a clinician. If the data reveals a trend toward unhealthy diabetes management, healthcare professionals can notice it right away and update the patient’s treatment plan, without an appointment.
If this is all sounding a bit esoteric, perhaps an illustration of such management technologies would help to illuminate its practicality.
The Israeli startup GlucoMe, for example, combines cloud-based data analysis and stripped-down medical hardware in order to better address diabetes management. GlucoMe’s management platform combines a smart glucose monitor, an insulin pen monitor, a mobile app, and a cloud-based management system to help streamline treatment. GlucoMe’s “Digital Diabetes Clinic” leverages all the patient’s data gained from continuous use of the platform in order to recommend treatment programs for individuals, as well as manage larger populations of diabetics.
The monitor still uses a lancing device to measure blood glucose, but also analyzes it and communicates the information to the user’s smartphone via the company’s acoustic data transfer system. The data transfer doesn’t rely on WiFi or cellular data, enabling use of the platform in more remote areas. The system then relays the information to a healthcare professional, along with a recommended treatment plan.
“We won’t just tell you this patient is in a high glucose condition or a low glucose condition,” Ben Aharon, founder and CEO of GlucoMe, said in an interview with The Times of Israel. “It will analyze the data and recommend a full treatment plan.”
While the platform will be quite beneficial for individual patients and their practitioners to better manage treatment plans, the company’s hardware is only an enabler for data collection, according to Aharon. The cloud-based system could be used to more aptly manage diabetic populations like those receiving treatment at a single clinic, or everyone with the disease in a specific region. Algorithms and machine learning strategies can then be shared with healthcare providers to determine which patients may need further attention. The technology’s aim here is to discover which patients may only need digital intervention (like minor adjustments to medication plans), and which may need to physically see their healthcare provider—culminating in efficiency for clinicians and improving treatment for patients.
Thus far, GlucoMe has completed trials in the United States, Germany, and Israel, was awarded CE mark clearance in August 2016, and expects to win U.S. Food and Drug Administration (FDA) clearance this year.
Type 1 diabetes (as evidenced by the name) isn’t the only form of the disease, of course—it just presents more of a management challenge due to insulin dependency. In fact, 95 percent of diabetic patients have type 2 diabetes,1 and don’t necessarily require comprehensive management platforms like GlucoMe. Livongo Health (a consumer digital health company focused on chronic conditions), partnered with Voluntis (a company that develops therapeutic companion software with a focus on managing chronic conditions) in February to develop an insulin titration app that recommends basal insulin doses for patients with type 2 diabetes. Livongo’s cellular-enabled blood glucose meter leverages data science to provide personal insights and coaching based on real-time information. Combining this with Voluntis’ Insulia—which delivers automated basal insulin dose recommendations and educational coaching messages through a smartphone app—seeks to improve medication adherence and optimize management. That way, patients can avoid the potential adverse health effects arising from suboptimal medication use.
Closing the Technology Loop
The be all and end all of type 1 diabetes management technology is widely regarded to be something called a “closed loop system”—an automatic control system in which an operation, process, or mechanism is regulated by continuous feedback. In the context of diabetes, that continuous feedback takes the form of a continuous glucose monitor (CGM), such as those included in Dexcom’s G5 Mobile CGM System, Animas’ Vibe System, or Medtronic plc’s MiniMed series. To complete the analogy, the operation, process, or mechanism to be regulated would be the frequency and amount of insulin delivered by a pump, based on the CGM’s blood glucose readings.
So rather than patients sticking themselves multiple times a day to determine proper insulin dosage, a closed loop system does (most of) the work of measuring and dosing. Of course, the system can’t yet account for things like deviance in diet or exercise (which the patient would still have to input into the system) but it removes a great deal of the burden of responsibility for diabetic patients.
“The development of the MiniMed 670G system was motivated by our desire to help patients achieve better health and greater freedom,” explained Mike Hill, vice president of global marketing for intensive insulin management at global medical technology company Medtronic. “People with diabetes spend a significant amount of time managing their disease on a daily basis. While this doesn’t prohibit patients from living a normal life, it can be quite burdensome—mentally, physically, and emotionally. This latest advancement demonstrates our commitment to both improving clinical outcomes as well as simplifying diabetes management to improve quality of life. This is all made possible by the advancements made to our smart algorithms that enable greater glucose control with reduced patient input.”
Medtronic’s MiniMed 670G system, dubbed the world’s first approved hybrid closed loop system for insulin delivery, won its FDA nod in September 2016. It features an algorithm called SmartGuard HCL (for Hybrid Closed Loop) for therapy customization. Rather than a fully-closed loop system, a hybrid closed loop means the device modulates the user’s basal rate through micro-boluses. Closing this loop greatly reduces the stress on diabetics about figuring out their basal rate—with the technology diabetic patients and providers can focus their efforts on selecting the best level of automation to fit their management plan. The system’s glucose sensor also lasts for seven days, and contains diagnostic technology that monitors the sensor’s health.
“There is much interest among the diabetes community to increase the level of automation of diabetes technology solutions,” observed Hill. Of course, the system isn’t completely automated—patients still need to input certain sets of pertinent external data to ensure the most effective management plan.
“Our MiniMed 670G system, known as a hybrid closed loop system, still requires some interaction on the part of patients. Users of the system will need to enter mealtime carbohydrates, accept bolus correction recommendations, and periodically calibrate the sensor,” he continued. “The next step in our phased approach will focus on advancing our algorithm to enable automated correction boluses. Once this challenge is addressed, we will focus our efforts on automating meal-time boluses. The timing for development will be dependent upon on multiple variables, but we are committed to a phased approach that will increase the system’s ability to further automate certain tasks with the ultimate goal of developing a fully automated, closed loop system.”
Since MiniMed 670G was revealed, many have taken to dubbing the device the “artificial pancreas.” While MiniMed 670G’s intended function is to essentially mimic the function of the pancreas by delivering an insulin dose based on an algorithm derived from the patient’s pattern of blood glucose levels, misperceptions about what the term “artificial pancreas” means might lead to misinterpretations of the device’s function.
“To ensure clarity around Medtronic’s focus, we are moving away from using the term ‘artificial pancreas’ as perceptions around what that means varies,” Hill said. “Our focus is on increasing automation of our advanced insulin pump systems through smart algorithms that reduce the need for patient interaction and decision-making. We are working to transform diabetes care by taking a holistic approach that goes beyond devices, and uses informatics and integrated care to achieve real results for people living with diabetes. We know that every person’s journey with diabetes is unique, so we strive to understand their diverse needs and develop technologies that meet them.”
Of course, the MiniMed 670G isn’t the only device—though it was the first to gain FDA approval—with partial closed-loop capabilities. In December 2016, the FDA also approved the Animas (part of the Johnson & Johnson Diabetes Care companies) OneTouch Vibe insulin pump, which is integrated with Dexcom’s G5 Mobile CGM technology. This system requires a bit more participation on the part of the patient; blood glucose readings are collected by Dexcom’s sensor, sent to the insulin pump’s screen and compatible smart device, and the user is prompted to deliver the precise amount of insulin they would need from the pump.
Animas’ system is, however, the only integrated system approved for children as young as age 2. Parents and caregivers (up to five people in addition to the primary smart device, as specified by Dexcom’s app) can access their child’s blood glucose levels to make treatment choices.
“This system will offer kids living with diabetes a sense of freedom and will provide loved ones and caregivers with an insulin delivery and monitoring system that they can trust,” said John Wilson, worldwide vice president of insulin delivery for Animas Corporation.
Easing the Burden on Patients and Providers
Whether through constant feedback from a support group, a mobile management platform, or a device, closing the loop on care is the most promising avenue to ease the burden of diabetes management. Ideally, each of these tools would come together to form a personalized management plan that attacks the disease on multiple fronts.
Closed-loop technology relieves the burden of multiple daily blood glucose tests, and calculates recommended insulin dose—then either delivers it automatically or prompts initiation by the patient. Integrated management platforms help to close the loop between patients and their healthcare providers, enabling constant communication and transmission of blood glucose data to make tweaks in treatment in near-real-time, instead of through often laborious scheduling of clinic visits. Combining these tools with a network of support such as that provided by Beyond Type 1 or other similar diabetes support groups allows the constant feedback and subsequent adjustment that a true closed-loop system facilitates. All of these proactive tools can ultimately help to lessen the financial burden on patients by reducing the number of emergency visits due to spikes in blood glucose.
“The cost of diabetes to the healthcare system has been rising,” noted Hill. “In fact, the costs associated with hypoglycemia can be sizeable—with a single emergency service totaling $1,387 and a single inpatient service totaling $17,564.”
With digital health tools, anomalies in blood glucose levels could be resolved before they reach the critical point where an emergency room visit becomes necessary. In an ideal situation, there would be multiple lines of defense to prevent that costly trip to the hospital. A closed-loop technology would hopefully catch the anomaly first, administering the necessary amount of insulin to help stabilize glucose levels. The information would then either be communicated to a healthcare professional via the device, or a companion mobile health management tool. A short conversation with a healthcare provider would then determine whether a clinic visit is necessary or a resolution can be achieved from home.
Each of these tools—combined with inclusion in an online community—can converge to form a “closed-loop support system” for diabetes patients. It’s true that diabetes is a chronic condition requiring careful consideration of almost every aspect of the patient’s lifestyle, but it’s one that tens of millions of people manage every day—and those people are happy to loop patients in on the solutions that help them to thrive.
Reference
1 Centers for Disease Control and Prevention. National Diabetes Statistics Report: Estimates of Diabetes and Its Burden in the United States, 2014. Atlanta, GA: U.S. Department of Health and Human Services; 2014.