Ethicon11.20.20
In the longest-term study ever published on magnetic sphincter augmentation (MSA), Ethicon’s LINXReflux Management System was shown to provide effective long-term control of gastroesophageal reflux disease (GERD) and eliminated the need for daily reflux medications in 79% of patients.1 The study, which followed patients over a 6- to 12-year period, recently appeared in the journal Nature Scientific Reports.2
The LINX Reflux Management System is a flexible ring of small magnets placed around the lower part of the esophagus, the body’s natural barrier to reflux, during a minimally invasive procedure. The magnetic ring expands when a person ingests food and then contracts to prevent stomach contents, including gastric acid, from backing up into the esophagus and causing GERD, a condition that affects about 20% of people in the United States.3
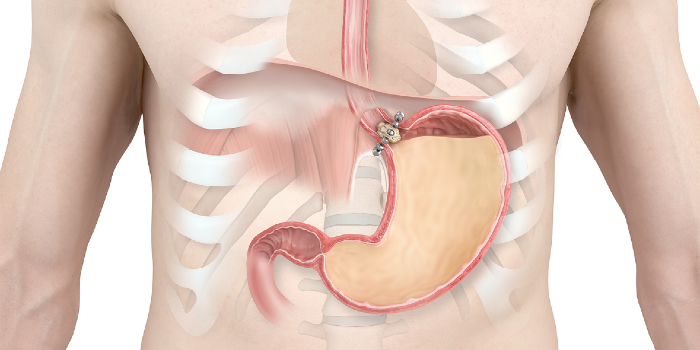
The LINX Reflux Management System expands when a person ingests food and then contracts to prevent stomach contents, including gastric acid, from backing up into the esophagus and causing GERD. Image courtesy of Ethicon.
The Study
In the single-center (IRCCS Policlinico San Donato in Italy) retrospective study of 335 patients who had an MSA procedure with LINX between 2007 and 2020, 124 patients who had been implanted for at least 6 years and up to 12 (median 9 years) were followed. Nearly 90% of LINX patients experienced long-term favorable outcomes defined as a greater than 50% improvement in their GERD-health related quality of life (GERD-HRQL) score and the discontinued use of proton pump inhibitors (PPIs), the current standard of care in medical therapy.4 There were no device erosions or migrations and only three instances (2.4%) of device removal due to either continued reflux symptoms, dysphagia or the need for an MRI in this long-term group.2 Patient satisfaction was 93.8% after 10 years.2
“Our new study corroborates the findings of previous studies but over a longer period of time, which is important for an implanted device,” said study co-author Luigi Bonavina, MD, professor of Surgery at University of Milan School of Medicine and chief of the Department of Surgery at IRCCS Policlinico San Donato. “The efficacy of the LINX System remained strong and the risk of complications did not increase many years after implantation. Based on these results and the high levels of patient satisfaction, MSA may represent a true paradigm shift that has the potential to fill the current therapy gap in GERD.”
This latest study builds on more than 50 peer-reviewed articles,5 including a randomized clinical trial, that show procedures with the LINX System are more effective than twice-daily PPIs in normalizing reflux6 and more effective in reducing disease-related payer cost 12 months post-surgery than laparoscopic Nissen fundoplication, a more invasive anti-reflux surgery.7
Several GI and surgical societies, including the American Society of General Surgeons (ASGS), Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), the American College of Gastroenterology (ACG) and the American Foregut Society (AFS), have issued consensus statements in favor of LINX procedures for appropriate GERD patients.
“Despite extensive clinical evidence, including this long-term study, and support from leading societies and academic centers, treatment with the LINX System remains out of reach for many patients due to inconsistent insurance coverage throughout the U.S.,” said Tom O’Brien, Worldwide Endomechanical president, Ethicon. “We are committed to providing the clinical and economic evidence that insurance carriers demand so patients with severe GERD can finally have access to the long-term relief they need and the potential for an improved quality of life wherever they happen to live.”
References:
1 Complete cessation of daily dose PPIs observed in 79% of patients at 9-year median follow up (n=124). Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020. 10(13753).
2 Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020;10(1):13753. doi:10.1038/s41598-020-70742-3.
3 El-Serag HB, Sweet S, Winchester C, et al. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2014. 63(6): 871-80. Poisson regression model of 16 studies yielded a sample size-weighted mean of 19.8% for the prevalence of GERD in the US.
4 Based upon a 6-12 years follow up study of 124 patients. Favorable outcomes were defined as ≥ 50% improvement in GERD-HRQL total score and PPI discontinuation. Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020. 10(13753).
5 https://www.americanforegutsociety.org/wp-content/uploads/2019/10/AFS-LINX-Final.pdf
6 Based on a RCT comparing patients on twice-daily PPI (BID PPI) to patients treated with laparoscopic MSA who all underwent impedance-pH testing. 91% of MSA patients vs. 58% of BID PPI patients had a normal number of reflux episodes at 6 months (p<0.001). Bell R, Lipham J, Louie B, et al. Laparoscopic magnetic sphincter augmentation versus double-dose proton pump inhibitors for management of moderate-to-severe regurgitation in GERD: A randomized controlled trial. 2018. Gastrointestinal Endoscopy.
7 Ayazi S, Zaidi AH, Zheng P, et al. Comparison of surgical payer costs and implication on the healthcare expenses between laparoscopic magnetic sphincter augmentation (MSA) and laparoscopic Nissen fundoplication (LNF) in a large healthcare system https://doi.org/10.1007/s00464-019-07021-4
The LINX Reflux Management System is a flexible ring of small magnets placed around the lower part of the esophagus, the body’s natural barrier to reflux, during a minimally invasive procedure. The magnetic ring expands when a person ingests food and then contracts to prevent stomach contents, including gastric acid, from backing up into the esophagus and causing GERD, a condition that affects about 20% of people in the United States.3

The LINX Reflux Management System expands when a person ingests food and then contracts to prevent stomach contents, including gastric acid, from backing up into the esophagus and causing GERD. Image courtesy of Ethicon.
The Study
In the single-center (IRCCS Policlinico San Donato in Italy) retrospective study of 335 patients who had an MSA procedure with LINX between 2007 and 2020, 124 patients who had been implanted for at least 6 years and up to 12 (median 9 years) were followed. Nearly 90% of LINX patients experienced long-term favorable outcomes defined as a greater than 50% improvement in their GERD-health related quality of life (GERD-HRQL) score and the discontinued use of proton pump inhibitors (PPIs), the current standard of care in medical therapy.4 There were no device erosions or migrations and only three instances (2.4%) of device removal due to either continued reflux symptoms, dysphagia or the need for an MRI in this long-term group.2 Patient satisfaction was 93.8% after 10 years.2
“Our new study corroborates the findings of previous studies but over a longer period of time, which is important for an implanted device,” said study co-author Luigi Bonavina, MD, professor of Surgery at University of Milan School of Medicine and chief of the Department of Surgery at IRCCS Policlinico San Donato. “The efficacy of the LINX System remained strong and the risk of complications did not increase many years after implantation. Based on these results and the high levels of patient satisfaction, MSA may represent a true paradigm shift that has the potential to fill the current therapy gap in GERD.”
This latest study builds on more than 50 peer-reviewed articles,5 including a randomized clinical trial, that show procedures with the LINX System are more effective than twice-daily PPIs in normalizing reflux6 and more effective in reducing disease-related payer cost 12 months post-surgery than laparoscopic Nissen fundoplication, a more invasive anti-reflux surgery.7
Several GI and surgical societies, including the American Society of General Surgeons (ASGS), Society of American Gastrointestinal and Endoscopic Surgeons (SAGES), the American College of Gastroenterology (ACG) and the American Foregut Society (AFS), have issued consensus statements in favor of LINX procedures for appropriate GERD patients.
“Despite extensive clinical evidence, including this long-term study, and support from leading societies and academic centers, treatment with the LINX System remains out of reach for many patients due to inconsistent insurance coverage throughout the U.S.,” said Tom O’Brien, Worldwide Endomechanical president, Ethicon. “We are committed to providing the clinical and economic evidence that insurance carriers demand so patients with severe GERD can finally have access to the long-term relief they need and the potential for an improved quality of life wherever they happen to live.”
References:
1 Complete cessation of daily dose PPIs observed in 79% of patients at 9-year median follow up (n=124). Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020. 10(13753).
2 Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020;10(1):13753. doi:10.1038/s41598-020-70742-3.
3 El-Serag HB, Sweet S, Winchester C, et al. Update on the epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut. 2014. 63(6): 871-80. Poisson regression model of 16 studies yielded a sample size-weighted mean of 19.8% for the prevalence of GERD in the US.
4 Based upon a 6-12 years follow up study of 124 patients. Favorable outcomes were defined as ≥ 50% improvement in GERD-HRQL total score and PPI discontinuation. Ferrari D, Asti E, Lazzari V, et al. Six to 12-year outcomes of magnetic sphincter augmentation for gastroesophageal reflux disease. Sci Rep. 2020. 10(13753).
5 https://www.americanforegutsociety.org/wp-content/uploads/2019/10/AFS-LINX-Final.pdf
6 Based on a RCT comparing patients on twice-daily PPI (BID PPI) to patients treated with laparoscopic MSA who all underwent impedance-pH testing. 91% of MSA patients vs. 58% of BID PPI patients had a normal number of reflux episodes at 6 months (p<0.001). Bell R, Lipham J, Louie B, et al. Laparoscopic magnetic sphincter augmentation versus double-dose proton pump inhibitors for management of moderate-to-severe regurgitation in GERD: A randomized controlled trial. 2018. Gastrointestinal Endoscopy.
7 Ayazi S, Zaidi AH, Zheng P, et al. Comparison of surgical payer costs and implication on the healthcare expenses between laparoscopic magnetic sphincter augmentation (MSA) and laparoscopic Nissen fundoplication (LNF) in a large healthcare system https://doi.org/10.1007/s00464-019-07021-4

























